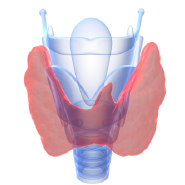
 The thyroid gland is a small, butterfly shaped organ in the lower neck which controls our metabolism by secreting thyroid hormone. A thyroid nodule is a lesion (adenoma, cyst, or tumor) within the thyroid gland. (The terms “thyroid lesion,“ “thyroid mass,” and “thyroid nodule” are used interchangeably.) These nodules are common, especially in women, and many patients have no symptoms. At times, patients can have symptoms of compression, such as difficulty breathing, swallowing or voice changes which can require surgery. Other nodules overproduce thyroid hormone, causing hyperthyroidism. The majority of thyroid nodules are benign (non-cancerous), but some are cancerous.
The thyroid gland is a small, butterfly shaped organ in the lower neck which controls our metabolism by secreting thyroid hormone. A thyroid nodule is a lesion (adenoma, cyst, or tumor) within the thyroid gland. (The terms “thyroid lesion,“ “thyroid mass,” and “thyroid nodule” are used interchangeably.) These nodules are common, especially in women, and many patients have no symptoms. At times, patients can have symptoms of compression, such as difficulty breathing, swallowing or voice changes which can require surgery. Other nodules overproduce thyroid hormone, causing hyperthyroidism. The majority of thyroid nodules are benign (non-cancerous), but some are cancerous.
Thyroid Nodules
- A thyroid nodule is a lump or growth inside of the thyroid gland. It may be benign (non-cancerous) or malignant (cancerous)
- Majority of thyroid nodules are benign (over 90%), which means that they are not cancers
- Most nodules in the thyroid gland are small and unlikely to be picked up on a physical exam or cause symptoms
- Thyroid nodules become more common with age
- 50% of people over age 65 have at least one thyroid nodule
- Most thyroid nodules are found on routine physical exams or by imaging done for unrelated reason, ie heart wise screening exams
- In children and teenagers, up to 20-30% of thyroid nodules can be cancerous
- Early stage thyroid cancer is painless and usually without any symptoms
Fine Needle Aspiration (FNA) of Thyroid Nodules
To find out if your thyroid nodule is benign or cancerous one usually begins with the Fine Needle Aspiration (FNA biopsy). Make sure that your doctor performs genetic testing and gives numbing medicine if needed for the thyroid nodule biopsy. Nodules in the thyroid that will likely be biopsied include:
- size greater than 1.5cm according to ATA (American Thyroid Association) guidelines
- suspicious ultrasound characteristics ( solid nodules, irregular borders, calcifications, nodule extending beyond the thyroid gland, shadowing of solid nodules)
- patient with family history of thyroid cancer or history of radiation exposure
- enlarging or painful nodules
- enlarged lymph nodes near the thyroid or in the neck area
*****PATIENTS WHO HAVE HAD A BIOPSY SHOWING FOLLICULAR CELLS OR FOLLICULAR NEOPLASM**** PLEASE READ THIS SECTION
As stated previously, the vast majority of thyroid nodules are benign….probably over 90% benign. YES even nodules with follicular cells!!! Therefore if you have a thyroid biopsy by another doctor or surgeon which shows follicular cells, this only means that the physician doing the FNA biopsy hit the thyroid gland. The normal thyroid is made up entirely of follicular cells, therefore ALL thyroid FNA biopsies should show some follicular cells assuming they biopsied the correct organ. PLEASE do NOT have surgery without genetic testing evaluation for these type of lesions/nodules as it can rule out cancers and an operation is NOT needed for diagnosis. If you are feeling pressured by your surgeon to have your thyroid removed for follicular lesion/ neoplasm to rule out a follicular cancer, it is VERY important to get a second opinion! Ask the doctor if the biopsy includes genetic evaluation if needed for your nodule before you go for consultation. It is also important to inquire if they use numbing medicine or lidocaine for the biopsy procedure. DO NOT let them tell you that “it is not needed”. In our opinion, these biopsies can be uncomfortable at times and we ALWAYS take the time to give local anesthesia or lidocaine to numb the skin before the biopsy.
Thyroid Goiter
A goiter is simply an abnormally enlarged thyroid gland. It may contain multiple nodules and can produce too much hormone (hyperthyroid), too little hormone (hypothyroid) or normal amount of hormone (euthyroid).
Most common causes:
- Multi-nodular goiter
- Grave’s Disease (patients are typically hyperthyroid)
- Hashimoto’s Disease
As goiters enlarge with time, they can cause difficulty breathing, swallowing problems, or voice changes. At times, goiters need to be removed surgically.
Thyroid Cancer
The incidence of thyroid cancer is increasing in the United States. In fact, thyroid cancer rates are rising faster than any other cancer in the United States. Thyroid cancer is now the fastest growing cancer worldwide! There are different types of thyroid cancer, including papillary, follicular, Hurthle cell, medullary, and anaplastic. Most thyroid cancers have an excellent prognosis and are not typically aggressive. Patients can be treated with minimally invasive surgery to remove these cancers and surrounding lymph nodes with smaller scars and easier recovery.
Symptoms that may appear in patients with thyroid cancer (remember that majority of patients do not have any symptoms and the thyroid blood tests are normal):
* large lymph node (swelling) in the neck that does not go away
* Hoarseness
* Difficulty breathing (especially when lying flat) or swallowing
* .Sensation of a “lump” when swallowing
* Unexplained throat clearing or cough
The primary treatment for almost all thyroid cancers is surgical removal or thyroidectomy. It is VERY important to have a surgeon who specializes in thyroid surgery performing these operations to lower risks of complications. Patients with thyroid cancer typically have an excellent prognosis after their operation. At times, patients will need therapy with radioactive iodine after surgery to treat their cancer. Long-term thyroid hormone replacement may also be necessary.
Graves’ Disease
Graves’ disease is an autoimmune process that causes the thyroid to overproduce thyroid hormone. It is more common in young women and can cause enlargement of the thyroid gland. Possible triggers for Graves’ Disease are thought to be viral or bacterial infection as well as a genetic link.
Symptoms of Graves’ hyperthyroidism:
- Muscle Weakness
- Irritability
- Tremor
- Thinning hair or hair loss
- Increased appetite
- Infertility
- Anxiety
- Emotional problems
- Difficulty concentrating
- Diarrhea
- Weight loss
- Problems sleeping
- Rapid heart rate
- Bulging eyes (exophthalmos)
How is it diagnosed?
- High free T3 or T4 (thyroxine) levels
- Low thyroid stimulating hormone (TSH) levels
- High levels of thyroid stimulating hormone (TSH) receptor antibodies
Graves’ disease can be treated with medications, radiation, or thyroid surgery.
Hashimoto’s Thyroiditis
Hashimoto’s thyroiditis is the most common inflammatory disease of the thyroid. It occurs when a patient’s own antibodies attack their thyroid gland. Hashimoto’s thyroiditis is more common in women ages 45-65, but can be seen in patients of any age. Hashimoto’s disease is also known as chronic lymphocytic thyroiditis.
Symptoms of Hashimoto’s Thyroiditis:
- Constipation
- Pale, dry skin
- Puffy face
- Increased sensitivity to cold
- Muscle aches
- Painful joints
- Prolonged menstrual bleeding
- Infertility
How is it diagnosed?
- Blood test for thyroid autoantibodies
- Elevated TSH (thyroid stimulating hormone)
- Firm, slightly enlarged, or even tender thyroid gland on exam
How is it treated?
- Thyroid replacement hormone for those with hypothyroidism
- Thyroid removal for patients with compressive symptoms or enlarging nodules
Parathyroid
The parathyroid glands are four small glands, each about the size of a grain of rice, located behind the thyroid gland. Their function is to regulate calcium metabolism in the body. Primary hyperparathyroidism is the disease process in which one or more of these glands overproduces PTH (parathyroid hormone). When this occurs, the calcium level in the body becomes too high. Left untreated, this disease can lead to osteoporosis, kidney disease, heart problems, depression, and fatigue.
Parathyroid glands monitor our calcium levels in the blood and bones. Sometimes one of the parathyroid glands will develop into a tumor which is known as hyperparathyroidism. “Hyper” means abnormally increased or excessive. It happens in almost 1 out of 100 people, most commonly in women over the age of 50. These parathyroid tumors will pull calcium out of the bones and raise the blood level of calcium. They do this by breaking down the bones which can lead to osteopenia or osteoporosis. High levels of calcium in the blood then can lead to fatigue, problems concentrating, high blood pressure, reflux, kidney stones, depression or even stroke. If your doctor ordered a blood calcium level and told you it was high, you have parathyroid disease until proven otherwise. After you have been told that your calcium is high, please make an appointment with Dr. Brady or Dr. Sabra with Austin Thyroid & Parathyroid Surgeons.
Primary hyperparathyroidism is caused usually by one gland that turns into a tumor or adenoma. It can happen in more than one of the parathyroid glands (15% of the time), this is why Dr. Brady and Dr. Sabra ALWAYS examine ALL four of your parathyroid glands in the operation. These tumors of the parathyroid are almost always BENIGN or not cancerous, but they can make patients feel awful. This is a list of common symptoms patients visiting Austin Thyroid & Parathyroid Surgeons complain of:
- Fatigue
- Brain fog
- Problems with memory or concentration
- Weakness and generalized lack of energy
- Dizziness
- Joint pain or muscle aches
- Kidney Stones
- Bone disease, osteoporosis or fractures
- High blood pressure
- Reflux or indigestion
- Depression, irritability or mood swings
- Problems sleeping
- Hair loss
- Irregular heart beat or arrhythmias or atrial fibrillation
PTH or parathyroid hormone is what the parathyroid glands secrete into the body which makes the bones leak calcium and increase the blood levels of calcium. If someone’s blood calcium is HIGH, their PTH level should be LOW. When both the calcium and PTH are high or elevated, then that patient has hyperparathyroidism and is a candidate for minimally invasive parathyroidectomy or MIP.
Minimally invasive parathyroid (MIP) surgery takes only about 15-20 minutes for Dr. Brady and Dr. Sabra to perform. All of our patients go home the SAME day with a small band-aid and a tiny incision (2cm or less than 1 inch) hidden in a natural skin crease on the neck. Nearly all of our patients have told us that they felt better in the recovery room or on the way home from the surgery center.
The most common cause (85%) of primary hyperparathyroidism is a single benign tumor called an adenoma. Approximately 15% of patients have 2 adenomas and less than 1% of patients have 4 gland hyperplasia (all glands enlarged).
All patients with this disease undergo “mini parathyroid surgery” which is minimally invasive and takes about 15-20 minutes to perform. Each of our patients get TWO(2) EXPERT parathyroid surgeons doing their operation to ensure the highest success rates. The surgery is safe, relatively painless, leaves a tiny scar, and is typically performed on an outpatient basis (No overnight stay in the hospital is necessary).
Secondary Hyperparathyroidism
Secondary Hyperparathyroidism is typically seen in chronic renal failure patients on dialysis. Failing kidneys are unable to convert vitamin D into its active form, which affects calcium levels. This, in turn, stimulates the parathyroid glands to overproduce PTH (parathyroid hormone).
Tertiary Hyperparathyroidism
Tertiary Hyperparathyroidism is a rare disease that is seen after kidney transplantation. The parathyroid glands continue to overproduce parathyroid hormone and patients sometimes require surgery to remove them.
Adrenal Gland
The adrenal gland is a small organ located above both kidneys that release hormones, including those in response to stress. The medulla (core) of the adrenal gland secretes epinephrine and norepinephrine, which are the adrenaline hormones. The cortex (outer portion) produces cortisol, aldosterone, and androgen hormones. Adrenal tumors can cause an over or underproduction of any of these hormones, which can cause a variety of symptoms for patients.
Examples of tumors of the adrenal gland
- Pheochromocytoma
- Aldosteronoma
- Adenoma
- Cyst
- Carcinoma
These lesions can be removed with a minimally invasive laparoscopic surgery using 3 small incisions and typically require only a one night stay in the hospital.
